Looking after your employees in the Health Care and Social Assistance industry
Reducing injuries in the Health and Social Care industry was identified as a national priority by Safe Work Australia1.
The Health Care and Social Assistance industry, including hospitals, Aged Care, Early Childhood and Disability Support, fulfil an essential role in caring for some of the frailest, most vulnerable members of our society. This industry is Australia’s largest and fastest growing industry, due to our growing as well as an ageing population2. The workers in this industry are diverse, coming from different cultural and linguistical background, with the majority comprising of young people starting their careers as well as those nearing retirement2.

Disturbing levels of work related injury in Care
Workers in the Health and Social Assistance industry share a passion of caring for people. Sadly due to the nature of work, the needs of clients, patients and residents are often prioritized over the wellbeing of the workers2. There is common conception that work cannot stop, with the work itself being both physically and emotionally demanding.

The dire result is an industry with the highest number of serious workers’ compensation claims Australia wide in 2019-20 and the second largest rise in claims (up 31% from the previous year)3. Workers’ compensation claims data from 2016/17 – 201/18 found that 43% of claim injuries are serious claims, resulting in five or more days off work.
Leading causes of injury
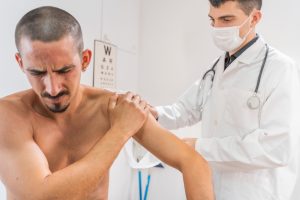
Workers’ compensation claims data from 2016/17 – 2017/18 found that the top causes of injury for the Health Care and Social Assistance industry were:
- Muscular stress (leading to musculoskeletal disorders (MSDs)
- Falls on the same level
- Work-related violence
- Psychosocial hazards including harassment and bullying
The data also found that the top injuries experience by the Health Care and Social Assistance industry were:
- Trauma to muscles, joints and ligaments
- Soft tissue injuries
- Anxiety / stress disorders
Reducing Musculoskeletal Injuries
Musculoskeletal Disorders (MSDs) is an injury to the body’s musculoskeletal system which includes sprains and strains of muscles, ligaments and joints. MSDs are most commonly caused by Hazardous Manual Tasks (HMTs) as well as slip, trip and falls. Injuries when moving patients continues to be a major issue for workers in the Care industry4.
Examples of HMT risk factors when handling and moving patients include:
- Repetitive or sustained force – long periods of patient handling task for more than 30 minutes at a time or more than two hours total per shift
- Awkward postures – prolonged or repeated postures when handling patients (such as bending forward or sideways, twisting, working at or below knee level)
- High or sudden force – for example when a carer attempt to catch a falling patient
- Repetitive movement – such as when adjusting wind-up or manual adjust beds

In the management of Hazardous Manual Tasks (HMT) employers need to be aware of research which shows lifting technique training, which continues to be used as a primary way to control HMT risks, is not effective in preventing MSDs5. This is because the risk factors are not removed, and that workers are still exposed to HMT hazards even when using safe lifting techniques.
Alarming levels of work related violence
Work related violence in the Care industry includes all incidents in which a health worker is abused, threatened or assaulted. It is manifested in two ways: external violence and service related violence.
Work related violence arises when health workers provide service to clients and patients. In the Care industry this consist of:
- Verbal aggression and threats – including language that is offensive, humiliating and discriminatory which may or may not involve shouting
- Throwing objects
- Striking, kicking, scratching, biting and spitting
- Physical intimidation and physical assault
- Threats with any type of weapon
Work related violence also include threatening or intimidating behaviour which occurs in writing, via text message or other forms of electronic communication.

Australian research has proved the existence of high rates of violence and aggression against health and care workers6,7. One study of health workers in NSW found:
- 47% had experienced an episode of violence within the past week
- 80% had experienced violence in the six months prior to completing the survey
- There was a reported injury rate of 28% as a result of work related violence
- Psychological injury was identified as the most common type of injury reported by participants.
The studies identified the areas with the highest risk as being the Emergency Department, Mental Health facilities as well as Aged Care.
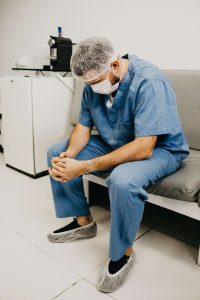
A collation of worldwide data performed in 2020 has also confirmed the serious rate of verbal and physical violence against healthcare workers8. It found that 62% of study participants had exposure to some form of workplace violence, 42% reported exposure to non-physical violence, and 24% experienced physical violence in the past year of the study.
Preventing injuries in the Health and Social Care Sector
Employers have an obligation under WHS laws to eliminate safety hazards in their organisation so far as is reasonably practicable. Healthcare employers need to review and install a safety management system in their workplace that strive to eliminate or isolate safety hazards to their workers. This includes policies and programs to protect their workers, mandatory training in safe work procedures, as well as ongoing support when workers experience an injury or work related violence.
All workers have the right to be safe in their workplace, and Care workers are no exception. Violence and aggression to health workers should never be an accepted part of the job. Instead, Care workers should be supported thoroughly in looking after their own health and safety. Looking after the wellbeing of employees is not only the right thing to do, but it also means they are able to better care for those in their charge.

Citations
- Safe Work Australia, 2018, ‘Health Care and Social Assistance: Priority Industry Snapshot’, accessed on 23 May 2022.
- NSW Government, ‘Health Care and Social Assistance – Work Health and Safety Sector Plan to 2022’, https://www.safework.nsw.gov.au/__data/assets/pdf_file/0008/555920/SW09276-Healthcare-and-assistance-WHS-sector-plan-to-2022.pdf, accessed on 23 May 2022.
- Final Australian Workers Compensation Statistics 2019-20, Safe Work Australia.
- WorkSafe Vic, ‘Transferring People Safely’, https://www.worksafe.vic.gov.au/resources/transferring-people-safely-handbook-workplaces, accessed on 30 May 2022.
- SafeWork NSW, ‘Effectiveness of Lifting Technique Training’, https://www.safework.nsw.gov.au/hazards-a-z/manual-tasks, accessed on 30 May 2022.
- Pich, J., 2019, ‘Violence in Nursing and Midwifery in NSW: Study Report’, NSW Nurses & Midwives Association, University of Technology Sydney.
- ACT Health, 2018, ‘Nurses and Midwives – Towards a Safer Culture’, ACT Government.
- Vento, S., Cainelli, F., Vallone, A., 2020, ‘Violence Against Healthcare Workers: A Worldwide Phenomenon With Serious Consequences’, Front Public Health, Vol 8, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7531183/ accessed on 31 May 2022.
- Australia Department of Health, 2018, ‘A Matter of Care Australia’s Aged Care Workforce Strategy’, Aged Care Workforce Strategy Taskforce.











